|
E. Linacre |
1/'99 |
Global climate change, as experienced during the past century and anticipated during the next, is largely due to human activities. The number of people on the Earth has risen from about one billion in 1800 AD, 2 in 1925, 3 in 1959, and 5.4 in 1996. The number is currently estimated to reach 7 to 9 billion by 2050, i.e. within the lifetime of many people already living. Governments worldwide are urged to take initiatives that curb the emission rate of greenhouse gases. This is a daunting challenge since the emission rate is proportional to the population.
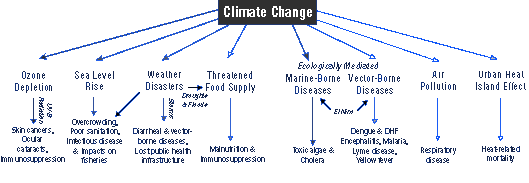
Global warming can affect human health is a variety of ways, as shown below.

The globe is estimated to be about 1K warmer in 2050 than in 1990. This would expose 600 to 800 million more people to the risk of malaria and 150-200 million more to dengue fever (1). Control measures in developed countries would cope with the increased risk. But the impact would be appreciable in areas where the diseases are already endemic, notably the eastern highlands of Africa, the Andes and the western mountains of China. Developing countries are most vulnerable because of continued urbanisation, few social resources and poor current health.
It is estimated that by 2030 the incidence of tropical diseases in Eastern Australia will have spread from Queensland to southern NSW (2). Diseases and pests in question include cattle tick, fruit fly, Ross River virus, paralysis tick, blue tongue virus and blowfly (affecting sheep) and cane toads. Biting midge, for instance, had been confined to the coastal region north of Rockhampton, but now occurs around Brisbane and may soon be found in Sydney
It is probable that stratospheric ozone depletion will peak around 2000, but the peak incidence of skin cancer will occur 50 years later, since it results from a cumulative exposure to UV-B. For instance, the increase of the cancer incidence by 2050 is likely to be 50% for Holland and 140% for Australia.
Asthma
The effect of warming on total and respiratory death rates is greater where temperatures are already above the comfort range of 16- 23ºC. There a rise by 1K increases respiratory mortality by 10%. Most common amongst respiratory diseases, asthma is clearly related to climate.
Epidemics of this disease in Melbourne, Australia, have been found to be linked to the quantity of starch granules from allergenic rye-grass pollen (3). Another allergen is a weed called pellitory (Purietaria judaica) whose proliferation is likely to be affected by climate.
Also, asthma there is more common in Australia during summers with above-normal rainfall (4). About 80% of asthmatics in coastal populations are affected by house mites which rely on humid, warm conditions. Asthma is highly prevalent in cities such as Brisbane, Auckland (New Zealand), Durban (South Africa), Hong Kong and New Orleans, cities which have a summer mean temperature over 24°C and an average annual rainfall of over 100 cm (5).
Asthma may also be affected by ozone, which is results from photochemical reactions in the urban boundary layer, especially in summer, and also from thunderstorms and lightning. Ozone is a significant pulmonary irritant, however its actual effects upon asthma are unknown.
Asthma is rarely fatal, but each asthmatic person costs about $770 annually to the community, i.e. over $200 million annually in Australia. It is thus important to determine how climate change might affect prevalence of a disease already common in Australia (4).
References
(1) Martens, P. 1998. Climate Change and Health. (Earthscan, London).
(2) Sutherst, R.W. 1990. Impact of climate change on pests and diseases in Australia. Search, 21, 230-2.
(3) Beggs, P. 1996. Australia pays the health price of global climate change. Australian Medicine, 8, 12-3.
(4) Ewan, C., E. Bryant and D. Calvert 1991. Health Implications of Longterm Climatic Change (Aust. Gov. Publishing Service, Canberra).
(5) Derrick, E.H., 1972. Asthma and the Brisbane Climate. Aust. N.Z. Med.,13, 235-246.